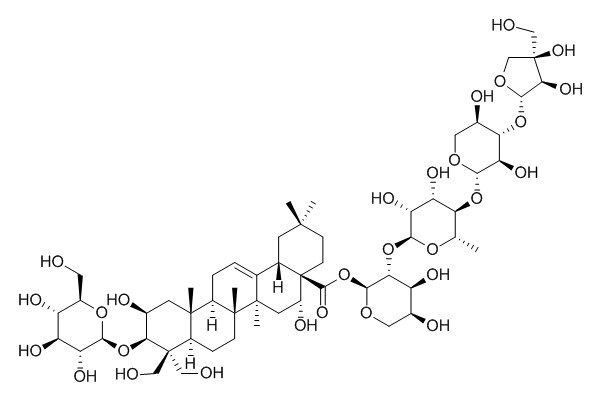
Platycodin D
Platycodon D shows antinociceptive, and anti-inflammatory activities, it can induce autophagy in NCI-H460 and A549 cells through inhibiting PI3K/Akt/mTOR signaling pathway and activating JNK and p38 MAPK signaling pathways. Platycodon D can inhibit migration, invasion, and growth of MDA-MB-231 human breast cancer cells via suppression of EGFR-mediated Akt and MAPK pathways. Platycodin D is also a potent adjuvant of specific cellular and humoral immune responses against recombinant hepatitis B antigen.
Inquire / Order:
manager@chemfaces.com
Technical Inquiries:
service@chemfaces.com
Tel:
+86-27-84237783
Fax:
+86-27-84254680
Address:
1 Building, No. 83, CheCheng Rd., Wuhan Economic and Technological Development Zone, Wuhan, Hubei 430056, PRC
Providing storage is as stated on the product vial and the vial is kept tightly sealed, the product can be stored for up to
24 months(2-8C).
Wherever possible, you should prepare and use solutions on the same day. However, if you need to make up stock solutions in advance, we recommend that you store the solution as aliquots in tightly sealed vials at -20C. Generally, these will be useable for up to two weeks. Before use, and prior to opening the vial we recommend that you allow your product to equilibrate to room temperature for at least 1 hour.
Need more advice on solubility, usage and handling? Please email to: service@chemfaces.com
The packaging of the product may have turned upside down during transportation, resulting in the natural compounds adhering to the neck or cap of the vial. take the vial out of its packaging and gently shake to let the compounds fall to the bottom of the vial. for liquid products, centrifuge at 200-500 RPM to gather the liquid at the bottom of the vial. try to avoid loss or contamination during handling.
Mol Med Rep.2024, 29(2):26.
Asian J Beauty Cosmetol2021, 19(1): 57-64.
Mol Immunol. 2016, 78:121-132
Trop J Pharm Res.2023, 22(3):283-288.
Biochem Pharmacol.2017, 130:10-20
Antioxidants (Basel).2020, 9(2):E120
Pathogens.2018, 7(3):E62
Front Plant Sci.2021, 12: 648426.
Cells.2024, 13(14):1229.
Eur J Pharm Sci.2016, 94:33-45
Related and Featured Products
Int Immunopharmacol. 2004 Aug;4(8):1039-49.
Platycodin D and D3 isolated from the root of Platycodon grandiflorum modulate the production of nitric oxide and secretion of TNF-alpha in activated RAW 264.7 cells.[Pubmed:
15222978]
Platycodon D (PD) and D3 (PD3) isolated from Platycodon grandiflorum has been previously reported to show anti-inflammatory activities in rats.
METHODS AND RESULTS:
In this study, the production of proinflammatory cytokines, nitric oxide (NO) and tumor necrosis factor-alpha (TNF-alpha) was examined in a macrophage like cell line, RAW 264.7 cells, in the presence of PD and PD3, oligosaccharide derivatives of oleanolic acid. RAW 264.7 cells activated with lipopolysaccharide (LPS; 1 microg/ml) and recombinant interferon-gamma (rIFN-gamma; 50 U/ml) were treated with various doses of PD and PD3 for 24 h. Supernatants were analyzed for the production of NO and TNF-alpha using Griess reagent and enzyme-linked immunosorbent assay (ELISA), respectively. NO was inhibited in a dose-dependent manner by PD and PD3 (IC50 of Platycodin D approximately 15 uM, IC50 PD3 approximately 55 uM). The expression of inducible NOS (iNOS) was inhibited by these compounds, as measured by Western blot analysis, as well as the expression of iNOS mRNA, as measured by Northern blot analysis. RAW 264.7 cells were treated at various times after LPS and activation with PD. Treatment with PD up to 8 h after activation showed significant inhibition of NO, indicating that early signal transduction of NOS synthesis may be inhibited by PD. In contrast to NO, secretion of TNF-alpha as well as expression of TNF-alpha mRNA was increased by PD and PD3. TNF-alpha secretion from RAW 264.7 cells was measured at various times after LPS and rIFN-gamma activation. Secretion of TNF-alpha was also increased up to 8 h postactivation, suggesting that PD may stimulate TNF-alpha synthesis or inhibit degradation of TNF-alpha mRNA. Oleanolic acid was without effect on both the production of NO and secretion of TNF-alpha.
CONCLUSIONS:
These data suggest a dichotomous regulation of these important proinflammatory mediators by PD and PD3.
Evid Based Complement Alternat Med. 2014;2014:954508.
The Effects of Platycodin D, a Saponin Purified from Platycodi Radix, on Collagen-Induced DBA/1J Mouse Rheumatoid Arthritis.[Pubmed:
24511322]
The object of this study is to observe the effects of Platycodin D, a saponin purified from Platycodi Radix, on mice collagen-induced arthritis (CIA).
METHODS AND RESULTS:
A daily dose of 200, 100, and 50 mg/kg Platycodin D was administered orally to male DBA/1J mice for 40 days after initial collagen immunization. To ascertain the effects administering the collagen booster, CIA-related features (including body weight, poly-arthritis, knee and paw thickness, and paw weight increase) was measured from histopathological changes in the spleen, left popliteal lymph node, third digit, and the knee joint regions. CIA-related bone and cartilage damage improved significantly in the Platycodin D-administered CIA mice. Additionally, myeloperoxidase (MPO) levels in the paw were reduced in Platycodin D-treated CIA mice compared to CIA control groups. The level of malondialdehyde (MDA), an indicator of oxidative stress, decreased in a dose-dependent manner in the Platycodin D group. Finally, the production of IL-6 and TNF- α , involved in rheumatoid arthritis pathogenesis, was suppressed by treatment with Platycodin D.
CONCLUSIONS:
Taken together, these results suggest that Platycodin D is a promising new effective antirheumatoid arthritis agent, exerting anti-inflammatory, antioxidative and immunomodulatory effects in CIA mice.
Int Immunopharmacol. 2015 Jul;27(1):138-47.
Platycodin D attenuates acute lung injury by suppressing apoptosis and inflammation in vivo and in vitro.[Pubmed:
25981110]
Platycodin D (PLD) is the major triterpene saponin in the root of Platycodon grandiflorum (Jacq.) with various pharmacological activities. The purpose of the present study was to evaluate the protective effects and possible mechanisms of PLD on acute lung injury (ALI) both in vivo and in vitro.
METHODS AND RESULTS:
In vivo, we used two ALI models, lipopolysaccharide (LPS)-induced ALI and bleomycin (BLE)-induced ALI to evaluate the protective effects and possible mechanisms of PLD. Female BALB/c mice were randomly divided into the following groups: control group, LPS group, LPS plus pre-treatment with dexamethasone (2 mg/kg) group, LPS plus pre-treatment with PLD groups (50 mg/kg, 100 mg/kg), LPS plus post-treatment with dexamethasone (2 mg/kg) group, LPS plus post-treatment with PLD groups (50 mg/kg, 100 mg/kg), BLE group, BLE plus pre-treatment with dexamethasone (2 mg/kg) group, BLE plus pre-treatment with PLD groups (50 mg/kg, 100 mg/kg), BLE plus post-treatment with dexamethasone (2 mg/kg) group, and BLE plus post-treatment with PLD groups (50 mg/kg, 100 mg/kg). PLD was orally administered before or after LPS or BLE challenge with mice. Mice were sacrificed, and lung tissues and bronchoalveolar fluid (BALF) were prepared for further analysis. Our results showed that PLD significantly decreased lung wet-to-dry weight ratio (lung W/D weight ratio), total leukocyte number and neutrophil percentage in the BALF, and myeloperoxidase (MPO) activity of lung in a dose-dependent manner. Besides, cytokine levels, including interleukin (IL)-6, tumor neurosis factor (TNF)-α were also found significantly inhibited in BALF. Furthermore, PLD effectively inhibited the expressions of nuclear factor κB (NF-κB), Caspase-3 and Bax in the lung tissues, as well as restored the expression of Bcl-2 in the lungs and improved the superoxide dismutase (SOD) activity in BALF. In vitro, we used LPS-challenged cell model to evaluate the protective effects and possible mechanisms of PLD. MLE-12 cells were stimulated with LPS in the presence and absence of PLD. The levels of TNF-α, IL-6 and the expressions of NF-κB, Caspase-3, and Bax were remarkably down-regulated, while the expression of bcl-2 was significantly up-regulated in PLD treatment groups in MLE-12 cells.
CONCLUSIONS:
These results showed that the administration of PLD improved ALI both in vivo and in vitro, possibly through suppressing apoptosis and inflammation.
Phytomedicine . 2019 Jan;52:254-263.
Platycodin D, a novel activator of AMP-activated protein kinase, attenuates obesity in db/db mice via regulation of adipogenesis and thermogenesis[Pubmed:
30599906]
Abstract
Background: Platycodi Radix (root of Platycodon grandiflorum) and its active compound Platycodin D (PD) has been previously shown to possess anti-obesity properties, but the underlying mechanisms remain poorly understood.
Purpose: The present study was aimed to evaluate the anti-obese effect of PD and reveal its mechanism of action.
Study design/methods: Genetically obese db/db mice were orally treated with PD for 4 weeks, and body weight gain, adipose tissue weight, serum parameters were measured. Then, assays on adipogenic factors, thermogenic factors, and AMP-activated protein kinase (AMPK) pathway were performed in PD-treated 3T3-L1 murine adipocytes, human adipose-derived mesenchymal stem cells (hAMSCs), and primary cultured brown adipocytes.
Results: PD treatment attenuated body weight gain, suppressed white adipose tissue weight and improved obesity-related serum parameters in db/db mice. Two major adipogenic factors, peroxisome proliferator-activated receptor gamma (PPARγ) and CCAAT/enhancer binding protein α (C/EBPα) were decreased by PD treatment in WAT of db/db mice, 3T3-L1 adipocytes and hAMSCs. In BAT of db/db mice and primary cultured brown adipocytes, PD treatment elevated the expressions of uncoupled protein 1 (UCP1) and peroxisome proliferator-activated receptor γ coactivator 1 α (PCG1α), the key regulators of BAT-associated thermogenesis. In addition, PD activated AMPKα both in vivo and in vitro. However, when AMPK was inhibited by compound C, PD treatment failed to suppress adipogenic factors and increase thermogenic factors.
Conclusions: PD improved obesity in db/db mice by AMPK-associated decrease of adipogenic markers including PPARγ and C/EBPα. PD increased thermogenic factors such as UCP1 and PGC1α in db/db mice and primary cultured brown adipocytes. AMPK inhibition nullified the effects of PD, suggesting its anti-adipogenic and thermogenic actions were dependent on AMPK pathway activation.
Keywords: AMP-activated protein kinase pathway; Adipogenesis; Obesity; Platycodin D; Thermogenesis.
J Cancer. 2015 May 23;6(7):623-31.
Platycodin-D Induced Autophagy in Non-Small Cell Lung Cancer Cells via PI3K/Akt/mTOR and MAPK Signaling Pathways.[Pubmed:
26078792 ]
Platycodin D (PD) is an effective triterpene saponin extracted from the root of Platycodon grandiflorum which has been used clinically to treat pulmonary diseases in traditional Chinese medicine. Recently, it has been reported that PD has anti-tumor effects in various cancer models through the induction of apoptosis. However, whether PD induces autophagy in both cell lines and its molecular mechanisms have not been elucidated.
METHODS AND RESULTS:
Here, our present study confirmed that PD induced autophagy in both NCI-H460 and A549 cells via up-regulating the expression levels of Atg-3, Atg-7 and Beclin-1. Meanwhile, PD contributed to the up-regulation of LC3-II at both protein and mRNA levels. Further detection of the PI3K/Akt/mTOR signaling pathway compared to LY294002 (PI3K kinase inhibitor), RAP (mTOR kinase inhibitor) and insulin (an activator of PI3K/Akt/mTOR signaling pathway) showed that PD induced autophagy through inhibiting the pathway at p-Akt (Ser473), p-p70S6K (Thr389) and p-4EBP1 (Thr37/46) in both cell lines. Moreover, the examination of MAPK signaling pathway showed that PD treatment increased the phosphorylation of JNK and p38 MAPK, while decreased the phosphorylation of Erk1/2 in both cell lines. Additionally, the effects assessed with a panel of pharmacologic inhibitors, including U0126 (Erk1/2 kinase inhibitor), SP600125 (JNK kinase inhibitor) and SB203580 (p38 MAPK kinase inhibitor) suggested that the activation of JNK and p38 MAPK participated in PD-induced autophagy.
CONCLUSIONS:
Taken together, these findings suggested that PD induced autophagy in NCI-H460 and A549 cells through inhibiting PI3K/Akt/mTOR signaling pathway and activating JNK and p38 MAPK signaling pathways. Therefore, PD may be an alternative compound for NSCLC therapy.
Planta Med. 2001 Jun;67(4):362-4.
Inhibition of prostaglandin E2 production by platycodin D isolated from the root of Platycodon grandiflorum.[Pubmed:
11458457 ]
METHODS AND RESULTS:
Platycodin D, isolated from the root of Platycodon grandiflorum A. DC. (Campanulaceae) suppressed prostaglandin E2 production at 10 and 30 microM in rat peritoneal macrophages stimulated by the protein kinase C activator 12-O-tetradecanoylphorbol 13-acetate (TPA). Platycodin D3 and oleanolic acid showed no effect at these concentrations. Western blot analysis revealed that the induction of COX-2 protein by TPA was inhibited by Platycodin D in parallel with the inhibition of prostaglandin E2 production.
CONCLUSIONS:
Platycodin D showed no direct effect on COX-1 and COX-2 activities. TPA-induced release of [3H]arachidonic acid from pre-labeled macrophages was also not inhibited by Platycodin D.
Eur J Pharmacol. 2006 May 10;537(1-3):1-11.
Platycodin D-induced apoptosis through nuclear factor-kappaB activation in immortalized keratinocytes.[Pubmed:
16631160 ]
Platycodi Radix is the root of Platycodon grandiflorum and it is widely used in the traditional Oriental medicine as an expectorant for pulmonary diseases and a remedy for respiratory disorders. Platycodin D is the major constituent of triterpene saponins in the root.
METHODS AND RESULTS:
This study investigates apoptosis by Platycodin D in immortalized human keratinocytes (HaCaT). Platycodin D-induced apoptosis in HaCaT cells was confirmed by DNA fragmentation, caspase-3 activation, and caspase-8 activation. Platycodin D could activate inhibitor of nuclear factor-kappaB kinase (IKK)-beta in the nuclear factor-kappaB (NF-kappaB) activation of upstream level, but not IKK-alpha. Pretreated-N-tosyl-l-phenylalanine chloromethyl ketone (TPCK), a potent NF-kappaB inhibitor, could suppress the induction of apoptosis and activation of NF-kappaB of HaCaT cells by Platycodin D. We also demonstrated that Platycodin D-mediated apoptosis of HaCaT cells upregulates Fas receptor and Fas ligand (FasL) expression, but did not exhibit p53 activation. HaCaT cells were also transfected with pFLF1, which preserves the promoter region of Fas receptor gene containing NF-kappaB binding site. On incubation with Platycodin D, the NF-kappaB activity related to Fas receptor increased in a dose-dependent manner. Among the major transcription elements on Fas receptor and FasL promoter, NF-kappaB activation was shown to have an essential role in the expression of the death receptor such as FasL.
CONCLUSIONS:
These results suggest that Platycodin D has the ability to induce apoptosis in HaCaT cells through the upregulation of Fas receptor and FasL expression via to NF-kappaB activation in the transcriptional level. These results demonstrate that the NF-kappaB activation plays a crucial role in the induction of apoptosis in human HaCaT cells on treatment with Platycodin D.
Vaccine. 2009 Jan 29;27(5):757-64.
Platycodin D is a potent adjuvant of specific cellular and humoral immune responses against recombinant hepatitis B antigen.[Pubmed:
19041358]
The ideal adjuvants for hepatitis B vaccines should be capable of eliciting both strong humoral and cellular immune responses, especially Th1 cell and cytotoxic T lymphocyte (CTL) responses. However, Alum used as adjuvants in the hepatitis B vaccines currently commercialized offers limitation in inducing cell-mediated response. Therefore, a less hemolytic saponin Platycodin D (PD) from the root of Platycodon grandiflorum has been explored for its potential as an alternative adjuvant.
METHODS AND RESULTS:
In order to compare the adjuvant activity with Alum, antigen-specific cellular and humoral immune responses were evaluated following immunization with a formulation containing hepatitis B surface antigen (HBsAg) adjuvanted with PD and Alum in mice. The Con A-, LPS-, and HBsAg-induced splenocyte proliferation and the serum HBsAg-specific IgG, IgG1, IgG2a, and IgG2b antibody titers in the HBsAg-immunized mice were significantly enhanced by PD (P<0.05, P<0.01 or P<0.001). PD also significantly promoted the production of Th1 (IL-2 and IFN-gamma) and Th2 (IL-10) cytokines and up-regulated the mRNA expression of Th1 cytokines (IL-2 and IFN-gamma) in splenocytes from the mice immunized with HBsAg (P<0.001). Besides, PD remarkably increased the killing activities of natural killer (NK) cells and CTLs from splenocytes in the HBsAg-immunized mice (P<0.001), which may have important implications for vaccination against hepatitis B virus.
CONCLUSIONS:
The results indicated that PD has strong potential to increase both cellular and humoral immune responses and elicit a balanced Th1/Th2 response against HBsAg, and that PD may be the candidates as adjuvants for use in prophylactic and therapeutic hepatitis B vaccine.
Am J Chin Med. 2004;32(2):257-68.
Antinociceptive profiles of platycodin D in the mouse.[Pubmed:
15315263]
Platycodin D (PD), one of several triterpene saponins, was isolated from roots of Platycodon grandiflorum. We previously reported that intracerebroventricular (i.c.v.) administration of PD showed an antinociceptive effect as measured by the tail-flick assay. However, its exact role in the regulation of antinociception in the various types of pain models has not yet been characterized. Thus, we attempted to find antinociceptive profiles of PD in various pain models.
METHODS AND RESULTS:
PD administered intraperitoneally (i.p.), i.c.v. or intrathecally (i.t.) showed antinociceptive effects in dose-dependent manners as measured by the tail-flick, writhing and formalin tests. In the tail-flick test, PD at the low doses reached the peak after 15 minutes and returned to the control level after 60 minutes. However, higher doses of PD showed a strong antinociception at least for 1 hour. PD administered i.t. showed stronger antinociception than that induced by i.c.v. administration PD in both tail-flick and writhing tests. In the formalin test, PD administered i.p., i.c.v. or i.t. showed antinociceptive effects during both the first (direct nociceptive stimulation) and second (late inflammatory) phases. Pretreatment with naltrexone i.p., i.c.v. or i.t. did not affect PD-induced inhibition of the tail-flick response.
CONCLUSIONS:
Our results suggest that PD shows a strong antinociceptive effect on the tail-flick, writhing and formalin tests, acting on central nervous system. However, PD-induced antinociception may not be mediated by the opioid receptors.